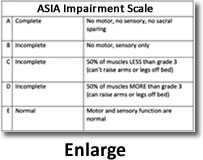
 Categories of SCI
Categories of SCIAcute effects
| Four Phases of Spinal Shock | |
Phase 1 - (0–24 h postinjury) |
The Deep Tendon Reflexes (DTR), ankle jerk and knee jerk are absent, but the bulbocavernosum reflex (BC), and the anal wink (AW), and the cremaster muscle (CM) reflexes may begin to recover. |
| Phase 2 - (1–3 days) initial reflex return, |
DTR are usually absent but the BC and CM may strengthen. According to, Ko, Ditunno, Graziani, and Little, the absence of all deep tendon reflexes after 24 hours is uncommon. |
| Phase 3: - (4 days to 1 month) early hyper-reflexia |
Most DTRs first reappear during this period, and they are evident in almost all subjects within 30 days. |
Phase 4 - (1–12 months) |
4 days–4 weeks: synapse growth, short axons and/or axon supplied; 1–12 months: synapse growth, long axons and soma supplied |
| Adapted from Ditunno, J., Little, J., Tessler, A. et al. Spinal shock revisited: a four-phase model. Spinal Cord 42, 383–395 (2004). https://doi.org/10.1038/sj.sc.3101603 | |
Immediately following significant spinal cord trauma, your patient may experience a temporary depression of sensation and spinal reflexes (spinal shock), below the level of the injury. During the period of spinal shock, the patient will exhibit some degree of flaccid paralysis, anesthesia, bowel and bladder dysfunction, and loss of reflex activity (Ziu, 2022). This can result in bladder and bowel incontinence, requiring patient-specific bladder and bowel management.
Spinal shock must be differentiated from Neurogenic shock, the terms are not interchangeable.
Neurogenic shock is a component of the spinal shock syndrome and refers to the hemodynamic instability seen in these patients with hypotension, bradycardia, and hypothermia (secondary to sympathetic-parasympathetic dysfunction/imbalance (Ziu, E. 2022).
An SCI can be, complete, incomplete or transient.
Neurogenic bladder
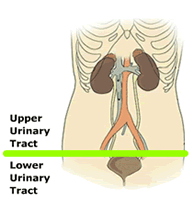 The term “neurogenic bladder” indicates lower urinary tract (LUT) dysfunction caused by neurological disease. LUT dysfunction is commonly reported by patients with neurological disease, and significantly impacts their quality of life (Meyer, 2019). After SCI, the heterogeneous presentation of LUT symptoms and dysfunction reflect the complexity of the neural control of the LUT, and the site of lesion in the neurological axis. (Panicker, J. N. (2020).
The term “neurogenic bladder” indicates lower urinary tract (LUT) dysfunction caused by neurological disease. LUT dysfunction is commonly reported by patients with neurological disease, and significantly impacts their quality of life (Meyer, 2019). After SCI, the heterogeneous presentation of LUT symptoms and dysfunction reflect the complexity of the neural control of the LUT, and the site of lesion in the neurological axis. (Panicker, J. N. (2020).
Although there are many possible effects of SCI on the urinary system, they all involve some combination of changes in muscle activity or sensation. The muscles involved can be the detrusor muscle of the bladder, the smooth muscle of the internal sphincter, the striated muscle of the external sphincter, and/or the urethra. Changes in sensation can involve the bladder and/or the urethra. Reflexes usually return below the level of injury. Over time, some reflexes even become hyperactive when the inhibitory effects of the higher neuro function is lost.
 We can classify spinal cord
injuries according to location of the lesion, and we can make some generalizations
about an SCI's effect on the urinary system.
We can classify spinal cord
injuries according to location of the lesion, and we can make some generalizations
about an SCI's effect on the urinary system.
A bladder that is hyperreflexic is overactive. It tends to empty "automatically".
| Detrusor Overactivity (DO) in Patients With Traumatic Spinal Cord Injury (Wang, Z. 2021) | |
| Cervical | 79.5% |
| Thoracic (T1-T9) | 61% |
| Thoracic (T10-T12) | 35.2% |
| Lumbar | 35% |
| Conical cauda | 19.2% |
Reference
American Association of Neurological Surgeons (AANS) (n.d.). Spinal Cord Injury. Retrieved February 16, 2023, from https://www.aans.org/en/Patients/Neurosurgical-Conditions-and-Treatments/Spinal-Cord-Injury
Burns, S. (2009). Management of Urinary Problems Caused by Spinal Cord Injury. University of Washington. Accessed 1/20/2022 from https://sci.washington.edu/info/forums/reports/urinary_problems.asp
Ditunno, J., Little, J., Tessler, A. et al. Spinal shock revisited: a four-phase model. Spinal Cord 42, 383–395 (2004). https://doi.org/10.1038/sj.sc.3101603
Gajewski J.B., Schurch B., Hamid R., Averbeck M., Sakakibara R., Agrò EF., Dickinson T., Payne CK., Drake M.J., Haylen B.T. (n.d.). An international continence society (ICS) report on the terminology for adult neurogenic lower urinary tract dysfunction (ANLUTD). Neurourology and Urodynamics. Retrieved March 10, 2023, from https://pubmed.ncbi.nlm.nih.gov/29149505/
Panicker, J. N. (2020). Dysautonomia: Neurogenic Bladder: Epidemiology, Diagnosis, and Management. Seminars in Neurology, 40(5), 569-579. https://doi.org/10.1055/s-0040-1713876
Ko, H. Y. (2018). Revisit Spinal Shock: Pattern of Reflex Evolution during Spinal Shock. Korean J Neurotrauma 14(2):47-54. doi: 10.13004/kjnt.2018.14.2.47. Epub 2018 Oct 31. PMID: 30402418; PMCID: PMC6218357.
Myers, J. B., Lenherr, S. M., Stoffel, J. T., Elliott, S. P., Presson, A. P., Zhang, C., Rosenbluth, J., Jha, A., Patel, D. P., Welk, B., & Neurogenic Bladder Research Group (2019). Patient Reported Bladder Related Symptoms and Quality of Life after Spinal Cord Injury with Different Bladder Management Strategies. The Journal of urology, 202(3), 574–584. https://doi.org/10.1097/JU.0000000000000270
Powell, C. R. (2016). Not all neurogenic bladders are the same: A proposal for a new neurogenic bladder classification system. Translational Andrology and Urology. Retrieved March 14, 2023, from https://tau.amegroups.com/article/view/8975/9689
Spinal Cord Injury Facts and Figures at a Glance (n.d.). https://sci.washington.edu/info/forums/reports/urinary_problems.asp#how
U.S. Department of Health and Human Services (DHHS) (n.d.). Spinal Cord Injury. National Institute of Neurological Disorders and Stroke. Retrieved March 20, 2023, from https://www.ninds.nih.gov/health-information/disorders/spinal-cord-injury
Wang, Z., Deng, H., Li, X., & Liao, L. (2021). The Video-Urodynamic and Electrophysiological Characteristics in Patients With Traumatic Spinal Cord Injury. International neurourology journal, 25(4), 327–336. https://doi.org/10.5213/inj.2040376.188
Zare, A., Jahanshahi, A., Rahnama'i, M. S., Schipper, S., & van Koeveringe, G. A. (2019). The Role of the Periaqueductal Gray Matter in Lower Urinary Tract Function. Molecular neurobiology, 56(2), 920–934. https://doi.org/10.1007/s12035-018-1131-8
Ziu E, Mesfin FB. Spinal Shock. [Updated 2022 Mar 3]. In: StatPearls [Internet]. Treasure Island (FL): StatPearls Publishing; 2022 Jan-. Available from: https://www.ncbi.nlm.nih.gov/books/NBK448163/